|
Variety of clinical symptoms including fatigue, dizziness, palpations, pre-syncope.Caused by improper timing of atrial and ventricular contractions resulting in AV dyssynchrony and loss of atrial “kick”.A chest x-ray will usually help to confirm the diagnosis.If the paced QRS morphology changes from a LBBB pattern (indicating RV placement) to a RBBB pattern (indicating LV placement), this suggests that the electrode has eroded through the interventricular septum.A dislodged pacing lead may float around inside the right ventricle, intermittently “tickling” the myocardium and causing ventricular ectopics or runs of VT (in much the same way as the guide wire of a central line!), alternating with failure of capture.Some great cases of runaway pacemaker are discussed here.Application of a magnet can be life saving but definitive treatment requires replacement of the pacemaker.Paradoxically, there may be failure to capture - causing bradycardia - because the pacing spikes are very low in amplitude (due to the depleted battery voltage) and because at very high rates the ventricle may become refractory to stimulation.The pacemaker delivers paroxysms of pacing spikes at 200 bpm, which may provoke ventricular fibrillation.This potentially life-threatening malfunction of older-generation pacemakers is related to low battery voltage (e.g.These will also usually terminate with application of a magnet.The ventricular rate cannot exceed the pacemaker’s upper rate limit (usually 160-180 bpm).This misfiring leads to pacing at an inappropriately fast rate.Sensors may “misfire” in the presence of distracting stimuli such as vibrations, loud noises, fever, limb movement, hyperventilation or electrocautery (e.g.Modern pacemakers are programmed to allow increased heart rates in response to physiological stimuli such as exercise, tachypnoea, hypercapnia or acidaemia.May result in rate related ischaemia in the presences of IHD.Newer pacemakers contain programmed algorithms designed to terminate PMT.Can be terminated by slowing AV conduction e.g.Results in a paced tachycardia with the maximum rate limited by the pacemaker programming.The paced ventricular complex results in further retrograde conduction with retrograde p wave generation thus forming a continuous cycle.Caused by retrograde p waves being sensed as native atrial activity with subsequent ventricular pacing.PMT is a re-entry tachycardia in which the pacemaker forms the antegrade pathway with retrograde conduction occurring via the AV node.Also known as endless-loop tachycardia or pacemaker circus movement tachycardia.Several types of pacemaker associated dysrhythmias can occur including pacemaker-mediated tachycardia (PMT), sensor-induced tachycardia, runaway pacemaker, pacemaker-mediated Wenckebach AV block and lead dislodgement dysrhythmia. If the patient’s native heart rate is above the pacemaker threshold, no pacemaker activity is expected and therefore output failure and capture failure cannot be recognised on the ECG. Multiple causes including electrode displacement, wire fracture, electrolyte disturbance, MI or exit block.Failure to capture occurs when paced stimulus does not result in myocardial depolarisation.Multiple causes including oversensing, wire fracture, lead displacement, or interference.Results in decreased or absent pacemaker function. 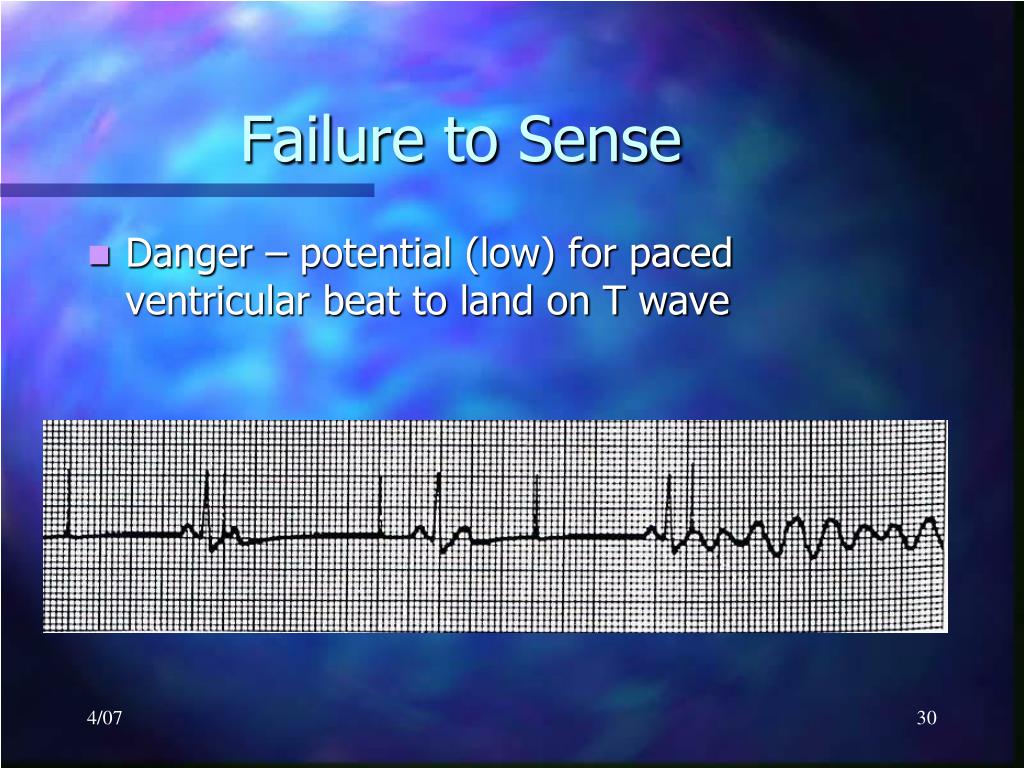
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
